An emerging best practice for behavioral health environments is to design spaces that minimize or eliminate areas where patients are secluded or restrained. The aim is to develop an environment designed to de-escalate, avoiding situations where medical staff need to physically intervene and restrain patients, which can be a traumatic act. Behavioral health environments often include seclusion rooms – either by design or in keeping with FGI code – to prevent patients from harming themselves or others. These rooms, which are sometimes padded, provide space for patients to de-escalate and calm.

Substance Abuse and Mental Health Services Administration’s (SAMHSA) Trauma and Justice Strategic Initiative set to define Trauma-informed Care (TiC). TiC recognizes and responds to the signs, symptoms, and risks of trauma to better support the health needs of patients who have experienced adverse childhood experiences and toxic stress.
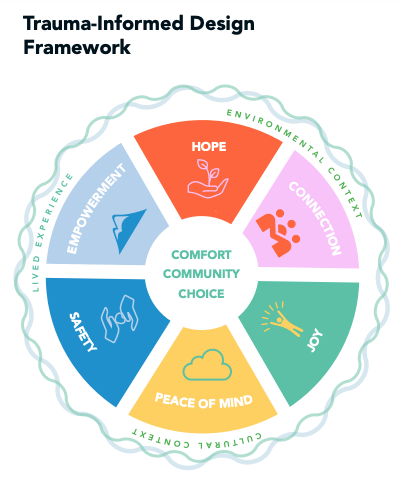
The 6 principles of TiC are:
- Safety
- Trustworthiness and Transparency
- Peer Support
- Collaboration and Mutuality
- Empowerment, Voice and Choice
- Recognizing Issues related to Cultural, Historical and Gender Identity
Evolved from these principles is the concept of trauma-informed design. Recognizing that the built environment has a profound impact on a person’s mood and behavior, designers need to create environments that are supportive, safe, calming and generally do not over stimulate a patient’s brain. When one thinks of the act of seclusion and restraint, it can be an incredibly traumatic experience.
The practice of designing to avoid seclusion helps patients feel safer, more respected, and more receptive to treatment within their environments. An environment which is normative, person-centered and therapuetic will set the stage for transformative mental health care. A healing environment will set the program for success and coupled with establishment of operational and observational protocols that allow staff to better anticipate escalation and deploy countermeasures which can diminish the frequency and severity of these occurrences, thereby minimizing the need for seclusion.
In this article, we’ll explore the key planning, operational and environmental considerations for designing in this manner.
Planning Considerations
Compartmentalization within a unit provides patients the space to self-regulate. A compartmentalized design allows staff to cordon off part of a unit and efficiently move patients out of that zone of risk when another patient begins to escalate. For example, in the design for CHKD’s Pediatric Behavioral Health Tower, 12-bed units are divided into four-room zones. These three zones each have cross-corridor doors, allowing staff to immediately observe if a patient is beginning to escalate within the zone. That visibility means that diffusing a situation is greatly simplified. As a patient begins exhibiting erratic behavior, staff can usher the other patients to a safe, adjacent zone and close the door behind them. This allows the escalating patient to interact with a durable environment as needed while staff work to calm that patient down.
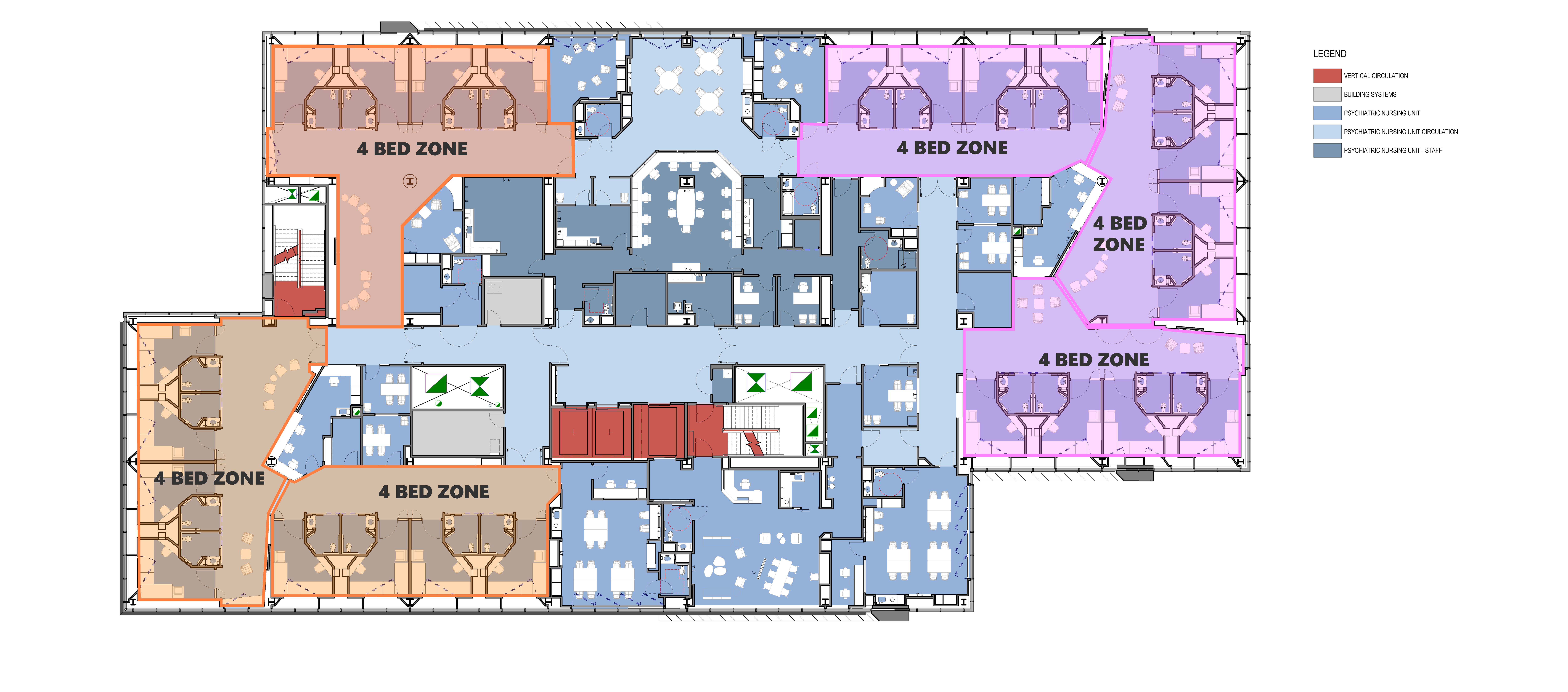
Another key planning consideration for designing to avoid seclusion is access. Doors should be designed to allow for access control from the team station or directly at the door, allowing staff to lock /unlock and move patient through the door as needed.
Staff’s access to Personal Protective Equipment (PPE) is also a critical consideration in this type of environment. In a unit with more free movement, anticipating where a patient might start acting aggressively (i.e. spitting or biting) would be impossible – so locating a PPE cabinet wouldn’t be an option. As an alternative, staff can use backpacks containing PPE such as face shields and Kevlar sleeves to help them protect themselves when they do need to intervene with patients.
Finally, providing dual means of egress from spaces where patients and staff interact is an important planning consideration. Having more than one way out allows staff members to feel safe when a patient acts aggressively or tries to corner them. Similarly, units should be equipped with a safe zone. Safe zones allow staff to retreat to a safe area in the event that a situation within a unit becomes unmanageable. These are typically located at the team center.
Operational Considerations
Staff buy-in is crucial for operating in this manner. Health system providers must believe in the philosophy of avoiding seclusion and remain committed to the model by maintaining keen observation of patients and removing interventional measures that would lead to that practice. Most patients can be re-directed before they escalate to a point of self-harm or aggression toward others, the key is encouraging your staff to interact with patients and not to “hang out” in the Team centers.
According to SAMHSA, 50 to 150 individuals die each year as a result of seclusion and restraint practices, while many others are injured or traumatize as a result of these events. What’s more, staff can also experience trauma and are put in danger by seclusion and restraint. Indoctrinating a philosophy of avoiding seclusion among staff should prove straightforward in light of these facts.

Right-sizing units to avoid overcrowding and optimize staffing for this model is also important. For example, a 36-bed unit is congested and noisy thus increasing the potential for conflict and negative response. A smaller unit with more direct clinical staff ratios decreases that risk. For a pediatric behavioral health environment, a 12-16 bed unit is optimal based on 1:3 or 1:4 staffing ratios. Some specialized neurological units, such as ones with lower functioning ASD patients, may have staffing as high at 4:1.
Environmental Considerations
Chiefly important to this model is the durability of materials within the environment. In a typical healthcare environment, designers would specify more durable materials in areas where a patient might be alone such as the patient’s room or toilet. In an area designated for staff members, designers can usually back off on durability. However, in an environment with more freedom of movement and in which patients will self-regulate, it requires a high level of construction and material durability in all areas where patients will be. As a result, designing in this manner does increase costs, but the benefits are considerable. A design that avoids seclusion provides patients the freedom they need to express frustration, decreases the need to medicate and can eliminate the need for restraint.
Calming elements and positive distractions also benefit this model. Sensory and tactile elements, color changing lighting, pleasing imagery and other calming elements can help redirect negative energy. These elements empower patients with sensory interventions that help prevent negative behaviors, i.e. self-harm, by enabling them to access appeasing elements that are conducive to self-regulating behaviors. Acoustics also plays an important role. Environments with hard surfaces required for durability tend to be noise reflective have been shown to increase anxiety. At Children’s Hospital of the Kings Daughter’s, our team angled interior walls to decrease reverberation, and selected materials such as cushioned back seem less flooring that were more absorptive facilitating a calmer, less noisy environment.

Trauma-informed design principles encompass environmental features such as: aesthetics, art, furniture, color, spatial organization and lighting/daylighting. Spaces should be visually interesting but not too busy. Spaces need to be well organized and provide the opportunity for patients to inhabit the space on their terms, for example, some patients prefer to sit around the edges or observe the space fully before entering. Artwork and color play a significant role in impacting mood and behavior, these environments should avoid deeply hued warm colors in favor of colors such as blues and greens that are more calming. Art inspired by nature can provide a great way to bring the outside in as well as to provide a connection to home that may be familiar or assist with wayfinding. Select landscapes and other imagery that is understandable and avoid images that are abstract or symbolic that could elicit a negative response. A balance of lighter spaces that appear more open is also important, but designers should try to avoid stark white spaces as these are reminiscent of institutional settings.
When considering furniture, features such as durability, cleanability and comfort need to be balanced. We prefer furniture that can be moved so that patients have some ability to modify their setting which provides a sense of control and independence. Having options is important as well, sociopetal arrangements can promote social interaction, but some patients may prefer to be by themselves in a quieter contemplative setting. Finally, lighting has a profound impact on how a space is perceived, so well-lit spaces are essential. Natural light from larger windows help to make a space feel light, bright and happy. We also look to provide patients with a reading light or color changing light to allow them have control over their own environment. At CHKD, there is color changing downlighting positioned over each bed with a patient selectable color range controller on the wall.

In Summary
Designing to avoid seclusion in behavioral health environments is a natural evolution in delivering more humane and effective care to patients and promotes the concepts of Trauma Informed Design. Careful planning, including zoned unit design, staff access to PPE, and providing two means of egress within units can help support this practice. Operationally, achieving leadership alignment in care philosophy and rightsizing patient units is also important. Finally, in the patient environment, durable materials and calming elements and helps patients self-regulate safely.
This article was authored by Jon Sell, a former employee of Array.
Explore Array’s design process for Children’s Hospital of the Kings’ Daughters in our AIA webinar.
{{cta(‘4494a350-501a-4d6a-85f1-a13272ac9b83’)}}




