In a previous post, I described how my mother’s battles with cancer led me to see healthcare environments differently. That journey really made me reflect on my design approach and made me want to design spaces in a new way. My dad’s recent patient experience with a cardiac ablation procedure further solidified my desire to change the face of healthcare design and dive a bit deeper into the processes our design can help support.

Monday, June 29th
5:15 AM
Leave house
5:45 AM
Arrive at Hospital and find parking
5:55 AM
Sign in at main registration
6:15 AM
We are called up to registration desk and receive wristbands. Registrar used alcohol wipes on everything, including the pen, before signing consents. Some of them are paper some are on an iPad. Scanned copies of DNR and RXs are checked to make sure they were entered correctly from the pre-registration online form prior to coming to the hospital.
6:25 AM
We walk to escalator and go down one floor to the interventional radiology waiting. There is no one at the desk, so I call number on service phone left on desk. The nurse states they will be out to get us soon.
6:45 AM
They take dad and I back to prep.
7:15 AM
Dad has the IV placed; all of his personal items are placed in a bag that I am now lugging around. He is on the stretcher waiting for the care team to do the rounds prior to the procedure. I go and find a chair to sit in. He is getting very impatient.
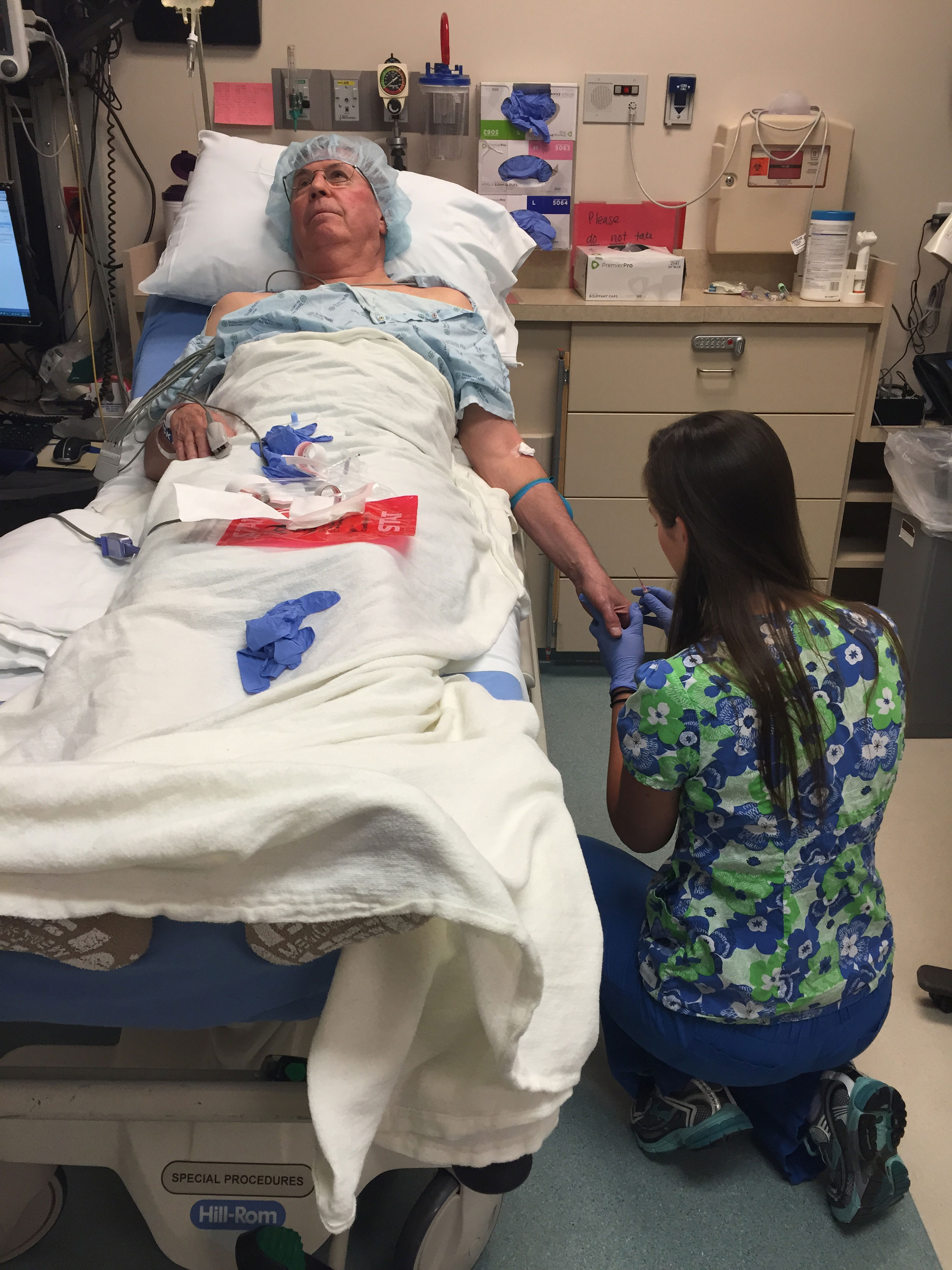
7:30 AM
A nurse comes to take vitals and realizes the electronic bed board is not working. There’s a little commotion as care team struggles to figure out who will go to what procedure room.
8:00 AM
The doctor and an anesthesiologist visit with my Dad, and tell transport that he is ready to go back to the EP lab (Electrophysiology procedure room).
8:15 AM
Transport takes dad back to the EP lab. I go to the waiting room and set up laptop to work; Wi-Fi isn’t working, so I have to use my hot spot to connect and work. I forgot my phone charger so I may not get as much work done as I hoped.
9:00 AM
Receptionist (who is now at the desk) tells me that the first part of the procedure went well and they are proceeding with the rest of the Ablation.
10:30 AM
Doctor comes to the waiting room in his scrubs and apron, sits in the chair next to me (not making use of the three consult-rooms that are directly adjacent to waiting) and tells me – in front of other families – that the procedure went well. However, they did have to “shock him back” a few times. He should be in recovery shortly and then I can go see him. I was a bit alarmed. He said it was no big deal.
 11:55 AM
11:55 AM
A nurse brings me back to recovery; Dad is one of two patients in recovery. He is complaining of pain and anxiousness. The nurse lets me know we are waiting on an empty patient room and it may be awhile, so she suggests I go get lunch and she will give my dad something to calm him. She will be watching my dad as well as the other patient only.
12:35 PM
I come back to recovery after eating a quick lunch. Dad is feeling better but needs to use the restroom. The nurse tells him he can’t move and must lay completely still until 5 PM – his movement is limited to turning his neck and moving his arms. The nurse now has three patients all waiting for inpatient beds – she hands my dad a urinal and closes the curtain.
12:40 PM
Another nurse and two more patients arrive into recovery. It becomes a little chaotic. I help dad with the urinal because the nurses are all too busy. Family isn’t supposed to be back in recovery, but they let me stay because they knew dad would be waiting a while. And, I think they were a little short staffed with patients being backed up waiting for beds.
1:00 PM
Dad is hungry but because he can’t move, the only food we can get is something I can feed to him laying down. The nurse tells us food service will take 45 minutes – so I decide to go to the cafeteria to see if can find something quickly. I come back with pudding and cottage cheese. I feed dad some of both, along with ice chips.
2:15 PM
We finally hear that a room is empty for dad, but it’s still being cleaned.
3:15 PM
We are finally taken to the patient room on the third floor cardiac unit. The nurse ends up transporting us both to the inpatient bed because the transport team is now off duty.
 3:30 PM
3:30 PM
All care team members have been in to see dad and take his vitals. He is getting very antsy because he can’t move and feels like he is being tortured.
5:00 PM on the dot
Dad hits the nurse call so he can get out of bed. The nurse comes in and helps dad out of bed and into a chair. I order him dinner, which will come in 45 minutes.
5:30 PM
Dad’s dinner arrives. He eats and then has a stomach ache from eating so much so fast (he had not eaten in 24 hours). He’s also concerned because he hasn’t had his normal meds for the day. He had a list printed of all his meds and when he takes them. I end up showing it to about three different people before we finally get an answer. The doctor hadn’t ordered all of the medications. The nurse will call the doctor to see what he wants to do.
6:30 PM
We finally get dad’s meds and he takes them.
7:15 PM
Shift change
I stay for the shift change to meet the night nurse. Dad has been up and down to the restroom and is watching a golf tournament on TV. I leave for the night to get some rest and feed the cat.
The next day and days following, I did get to take dad home and help him recover. The procedure at this time seems to have helped dissipate the symptoms of atrial fibrillation. While I am glad I could be present and help my father through this procedure, it did bring to light that the experience we often map for patients and families as we are designing spaces is so hard to predict and control if the caregivers don’t have the support and technology they need.
If the problems from inefficient scheduling of procedure rooms and backed up inpatient bed turn over so directly affected our 24-hour stay at a facility, imagine how that can be compounded over weeks, and months with many encountering what my father and I did. The staff was gracious, caring, and attentive. As we often find, they are overcoming so many daily obstacles to give the best care they can, probably with little thought to the space they were providing the care in.
As we continue to work as design professionals, and become patients or caregivers for loved ones’, we must keep in mind always that what we do should ultimately be invisible and not pointed to as why these healthcare professionals can do their job but perhaps why they do not have to think about it. I also hope that as our world is ever changing due to technology that we challenge our clients and ourselves for what the right answers are to support what they need to do on a daily basis.
We often know what the ideal should be, but what should the norm be? What is practical and easy to replicate? What happens when technology breaks? The facility that my dad was lucky enough to receive treatment in a nationally recognized health system with beautiful facilities, but all the thoughtful decisions that a talented team of designers and architects made cannot make the space work when the processes have not had the same attention and care given to them. Let’s all accept the challenge to change this story.




